Keys to Happiness
Written by Holly Prestidge | Photos and video by Daniel Sangjib Min
Stori Key climbed into her dad’s lap and wrapped her arms tightly around his neck.
Moments before, she was sitting on the couch in her living room listening to her parents, Kevin and Nelisa Key, talk about the emotional roller coaster of the last few years of their lives. Kevin was diagnosed with end-stage renal failure at another health system in November 2023, then received a living-donor kidney transplant at the VCU Health Hume-Lee Transplant Center in July 2025.
Stori, age 7, sat quiet and still, hanging onto her parents’ every word. Sometimes she’d watch them intently from behind a pillow she was clutching that nearly covered her face. She’d grin sheepishly when they talked about how brave she was and how she’d learned to help her daddy with the in-home dialysis machines he used for a year and a half.
Other times, when her mother began to cry, she’d look away.

A national transplantation leader for nearly 70 years, Hume-Lee performed the first kidney transplant in Virginia in 1957. That effectively established the foundation of a robust system that today routinely performs nearly 600 organ transplants annually.
From a societal perspective, living donation is the key to bridging the gap between the large number of potential recipients we have and the paucity of donors.
Dhiren Kumar, M.D., transplant nephrologist and medical director of the living donor kidney transplant program, VCU Health Hume-Lee Transplant Center
Last year, Hume-Lee performed 569 organ transplants in 2025. Of those, 328 were kidneys.
One of those was for Kevin.
July marks one year since his transplant, and sitting in their Chesterfield County home, the Keys described lessons learned from the hardest journey they have ever faced. They also talked about angels who appeared when they needed them most.
Living Donor Legacy
April is National Donate Life Month, which was established to raise awareness about the need for organ, eye and tissue donations. It also celebrates and honors both living and deceased donors.
More than 100,000 people are currently on the national transplant list. For those in need of a kidney, the average wait time is three to six years. For those with rare blood types, prior failed transplants and antibodies, that wait can be even longer.
Hume-Lee cares for patients using advanced therapies that allow it to evaluate and treat individuals who may be turned down by other centers. Wait times at Hume-Lee are significantly shorter than the national average for deceased donor kidneys. It has also pioneered living donor transplants, which, in recent years, accounted for 12% to 16% of all kidney transplants at VCU Health.
Kidneys from healthy living donors have the best short- and long-term outcomes. They reduce recipients’ five-year mortality rates from 40% to less than 6%, require fewer medications, carry a lower risk of rejection, improve quality of life and are more cost-effective than dialysis.
Living donors also create a positive ripple effect; an individual with a living-donor kidney is successfully taken off the national waiting list, which means another individual in need moves up.
“Statistically speaking, these kidneys last the longest,” said Dhiren Kumar, M.D., transplant nephrologist and medical director of the living donor kidney transplant program. That’s about 15 to 20 years, though the kidneys can last longer if well taken care of.
“From a societal perspective, living donation is the key to bridging the gap between the large number of potential recipients we have and the paucity of donors,” Dr. Kumar said. “It’s a slam dunk.”
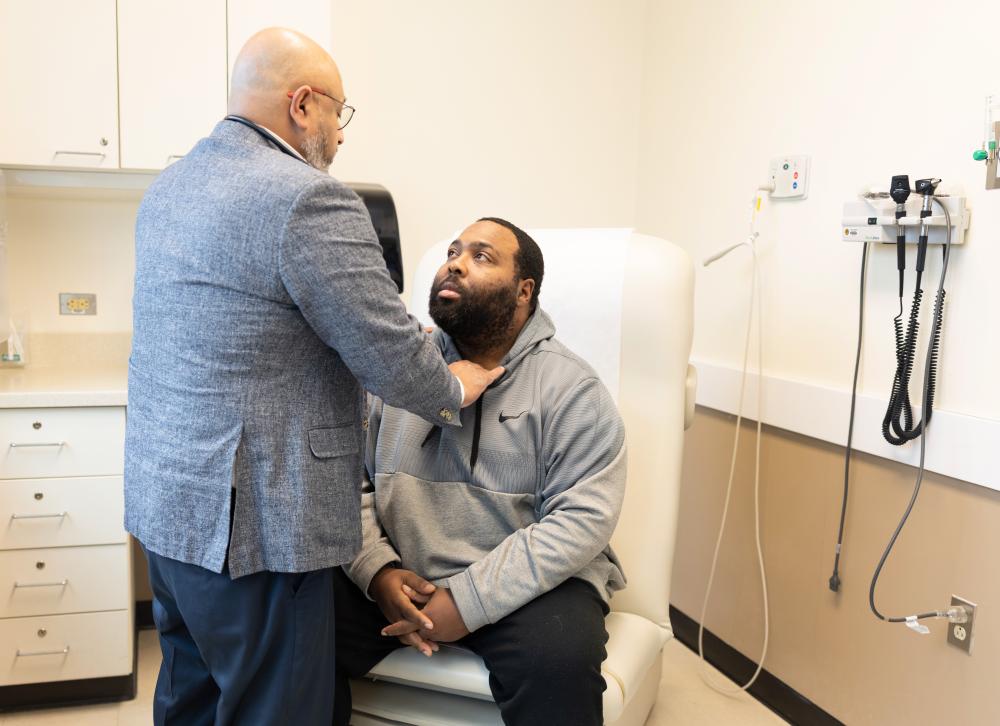
Family Ties
Kevin’s story began decades ago, when a doctor’s physical for middle school sports revealed issues with his kidneys. Back then it wasn’t alarming, and throughout high school and college, Kevin was routinely monitored by a nephrologist and took medications to keep things under control. By the time he met and married Nelisa, he was still monitoring his health.
Stori came along a few years later and life for this family of three was good.
The year 2023 changed everything.
Nelisa noticed subtle changes in her husband. He more easily tired, and his energy level dropped. Kevin chalked it up to getting older and taking care of an exuberant kindergartener. But by Thanksgiving, he was diagnosed with end-stage renal failure.
By one morning in January 2024, Kevin couldn’t make it down the 13 stairs in their home without stopping to catch his breath.
“He just wanted to go back upstairs and take a nap – he was begging to take a nap,” Nelisa said. The pleading scared her. She wondered if Kevin’s body was sending a message.
Something in her gut told her to keep him awake.
“I felt like God was saying something to me,” she said, her voice trailing off. “Like, if he closed his eyes, they wouldn’t open.”
At her urging, Kevin called his doctors and was told to come immediately to the hospital, where he was placed on emergency dialysis. Had he not sought help, he was told, he likely would have died within a week or two.
VCU Health took care of me every step of the way and went the extra mile to make sure I was okay before I was discharged.
Shaneé Simmons, living kidney transplant donor
From that moment, life revolved around Kevin’s dialysis, which consumed as many as 20 hours every week. While he started at a dialysis center, he later transitioned to using home dialysis so he could keep working. He’d work remotely from 8 a.m. to 5 p.m., then spend 4 hours on dialysis each weeknight. Nelisa’s social media is peppered with videos of sweet and sassy Stori helping her daddy with his dialysis routine – checking for bruises on his body and working any of the dozens of buttons required to run the machines.
On weekend nights, when Stori could stay up later than her normal bedtime, dialysis time became bonding time.
“She’d come down, get a blanket and just be right here next to me,” Kevin said.
Following his diagnosis, Kevin was placed on the transplant list, and friends and family immediately came forward to determine if they were potential donors. Kevin’s blood type was rare. His sister-in-law, Shaneé Simmons, shared the same type, though she was not initially considered a strong candidate for living donation by other transplant programs.
At least, not yet.
Dialysis went on, week after week, month after month. There was no news about potential donors.
In late 2024, Kevin learned from the home health care team who worked with him that individuals waiting for organ donations could list their cases with multiple hospitals.
Kevin sought out Hume-Lee. By the end of December, he was approved for a transplant largely because the one person who was rejected elsewhere as a living donor match for Kevin – his sister-in-law, Shaneé – was not only identified as a match but welcomed with open arms.
“A Perfect Match”
Maryland resident Shaneé Simmons loves her younger sister. Growing up, she and Nelisa and their mother were a close-knit trio. Shaneé explained that she and Nelisa have different fathers, and they weren’t close with them when they were young children.
“Seeing Kevin be a father to Stori is touching for me,” Shaneé said. “He’s a great man and a great father, and I told him from the very beginning, if he gets sick, I’ll be there.”
She also sees how Stori loves her dad, and she was willing to do whatever it took to make sure her niece – the name Stori was her suggestion, she proudly notes – has him around for a long time.
“I love my sister and I love Kevin, but in my heart, I did this for Stori,” Shaneé said. “My niece deserves that.”

Shaneé said once Hume-Lee approved her as a living-donor candidate, things suddenly got very real.
She was 41 and for the first time in her life, facing a complex surgical procedure. There may have been a moment or two of doubt, she said as she chuckled, such as those final moments before surgery when the enormity of the situation hit her.
“If you can get past the thought of death, everything else is a walk in the park,” she said. But her anxieties lessened when she learned about the entire team of people who would be watching over her every minute.
Donating an organ is a selfless act, and to honor those who do and make their experience more comfortable, most Hume-Lee living donors are taken care of in the Gumenick Suites following their surgery. It’s an area of VCU Medical Center’s main hospital that offers a level of personalized attention in a setting like that of a five-star hotel, with more nursing staff per patient and extra amenities like gourmet meals and accommodation for guests.
“VCU Health told me I was perfect,” Shaneé said regarding her status as a donor for Kevin. She was in the hospital for only a few days after surgery. Within about a week, she felt ready to go back to work.
“My experience was beautiful,” she said. “VCU Health took care of me every step of the way and went the extra mile to make sure I was okay before I was discharged.”
Dr. Kumar, from Kevin’s transplant team, said Hume-Lee is a transplant leader for three reasons: a decades-old foundation of patient-focused care, the insatiable drive to innovate, and the depth of expertise to overcome barriers.
“In transplantation, the possibilities are immense,” he said, explaining that the challenges of the past decades, such as early organ rejection rates have largely been addressed and now today’s issues involve making those transplanted organs last longer, maybe even to cover an entire lifetime. One transplant for life is now considered the holy grail of transplantation.
“From what we were doing a decade ago to what we’re doing now is completely different,” he said.
Hume-Lee launched robotic surgeries for transplant in 2014 and was the first transplant center on the East Coast to complete a successful robotic-assisted kidney implantation.
Robotic procedures involve surgeries performed by robotic arms and their instruments, which are controlled by surgeons at consoles on the other side of the room. It offers shorter recovery times, fewer complications for patients and better visualization for surgeons.
When I woke up that morning after surgery, it was like a new life, and it was the way life was supposed to be, like 4K, high definition right-in-your -face.
Kevin Key
Shaneé’s kidney was removed using the robotic approach.
“We are quite often the place where patients can turn when they have nowhere else to go, and we’re proud of that reputation,” said David Bruno, M.D., director of the Hume-Lee Transplant Center and chief of the Division of Transplant Surgery in the VCU School of Medicine.
“We lead innovation in transplantation through technological advancements, and we’re always focused on delivering the best possible outcomes for our very special community of patients,” he said, adding that transplant patients become VCU Health patients for life.
Dr. Kumar echoed those thoughts.
“We’re constantly evolving, seeing what is new, learning from other programs, doing research and presenting our data, and then other programs learn from us,” Dr. Kumar said. “The reason I’ve been here for nearly 20 years is because of the people I work with. I work with people who don’t think of obstacles as a wall where we stop. We see obstacles as challenges that we overcome as a team.”
Hume-Lee’s pioneering leaders laid the foundation decades ago for patient-focused care.
“That ethos has been going on for years and years and I think patients feel that and notice that in comparison to other centers,” Dr. Kumar said. “As you become a behemoth, there’s an almost protocol-driving efficiency built in, which doesn’t always translate into a personalized approach.
“But we are always cognizant of that, however much we grow we don’t want to lose that personal approach to patient care.”
There are days when Shaneé completely forgets she only has one kidney. Energetic, with a contagious laugh, she now moves through life deliberately when it comes to her health. She’s had to change her diet. She’s glad for the motivation to exercise.
She’s also proud of herself.
Lisa and Kevin never asked her to donate her kidney, Shaneé explained.
“I made that decision on my own, and I have no regrets,” she said. But she was surprised by how it made her feel.
“I felt heroic,” she said. “I’ve never felt like a hero, but, that day, I did.”
Her why is never far out of mind.
“I knew from the beginning that Kevin was a great man, and if I could save his life, that’s what I was going to do,” Shaneé said. She has a son but cares for Stori like her daughter.
“She’s my world.”
Stori Time
In a few months, the Keys will be heading off to Disney World. Mouse ears, fairy tale princesses and silliness are on the itinerary.
Stori turns 8.
Shaneé and Lisa can relax.
Kevin celebrates one year into his second chance at life, and it’s the first vacation the family has been able to take in a long time.
“Before surgery, I was here in the world, but there was a dimness,” Kevin said. “When I woke up that morning after surgery, it was like a new life, and it was the way life was supposed to be, like 4K, high definition right-in-your -face.”
Dr. Kumar said nothing in medicine quite compares to seeing patients after surgery and informing them that they’ll no longer need dialysis.
“The world that’s been closed to these patients on dialysis suddenly opens after a kidney transplant,” he said. “The cruises, the trips, that’s what living donations do for people.”
He continues to be awed by living donors.
“The gift of living donation is a sacrifice that not many people will understand,” Dr. Kumar said. “It’s life changing, but not just for the recipient. It means a daughter can go to Disney World with her dad and even after doing this for so long, it’s still tough for me to understand.”
He added: “Living donors are built differently, they think differently, and I’m glad to be serving them and be a conduit for their contribution and their sacrifices.”
Kevin credits Nelisa for being his angel at home, and he’s grateful to Shaneé beyond words.
“It really opened my eyes to see how much I was loved and how much my family supports me,” he said.
Kevin is aware that given his age, he may need another transplant years from now. He’s not afraid.
“If I ever have to go down that road again, I know I’m going to VCU Health and that I can trust them to help me through this process,” he said. “My doctors told me to trust them, and I did, and I’m feeling better and better every day.”
Kevin encourages anyone who can to consider becoming a living donor.
“I’m living proof that living-donor transplants not only saved my life, but my family’s lives as well,” he said. “I’m definitely going to make sure I do everything that I need to do to keep myself healthy so I can be around here for another 40 or 50 years.”
“I have way too much to live for.”

If you would like to support VCU Health Hume-Lee Transplant Center, please contact Andrew Hartley, senior director of Development, Integrated Care, at 804-869-0520 or aphartle@vcu.edu.
Your generosity saves lives.
Support patient care, education and research on the MCV Campus.