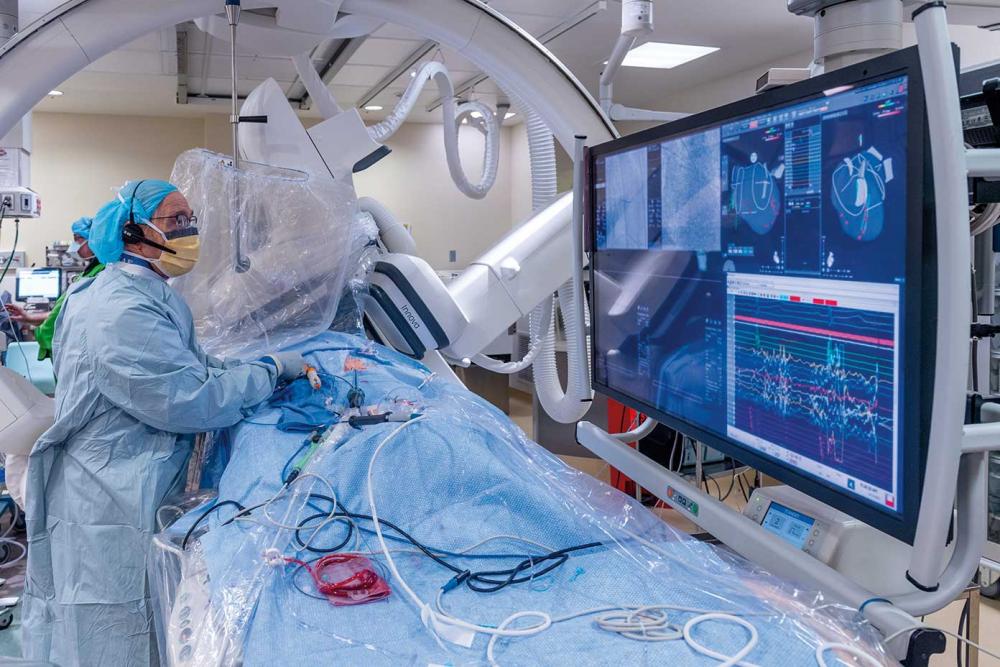
Remaining Active with Afib
Editor’s Note: This is an excerpt of a feature that appeared in the summer 2021 issue of NEXT magazine. Our online version includes the full article and more stories about innovative research happening on the MCV Campus.
***
Atrial fibrillation, or AFib, is the most common type of heart arrythmia in the U.S., and is expected to affect 12.1 million people across the country by 2030.
With symptoms that include lightheadedness, shortness of breath or fatigue, this abnormal heart rhythm occurs when the upper part of the heart — the atria — beats irregularly and too fast, causing the heart to quiver, or fibrillate. While the symptoms usually are not painful, AFib increases the risk of stroke five to seven times, and it is responsible for one in every four strokes that occur.
The Centers for Disease Control and Prevention reports that AFib was mentioned on 175,326 death certificates in 2018, and that AFib was the underlying cause of death in 25,845 of those cases.
For years, blood thinners have been used to prevent blood clots that lead to AFib-related strokes, while cardiac assist devices, catheter ablation procedures and a variety of minimally invasive approaches have been used to reset the rhythm or control the rate of the heart. And as a last resort, VCU Health and other institutions have offered surgical implantation of a device known as the WATCHMAN, which is permanently placed at the opening of the left atrial appendage.
Today, however, it looks as though the latest version of the WATCHMAN might actually be the best first solution and could free patients from having to take anticoagulants that thin blood and can cause serious bleeding problems — an especially concerning issue for those who would like to stay active as they advance in age.
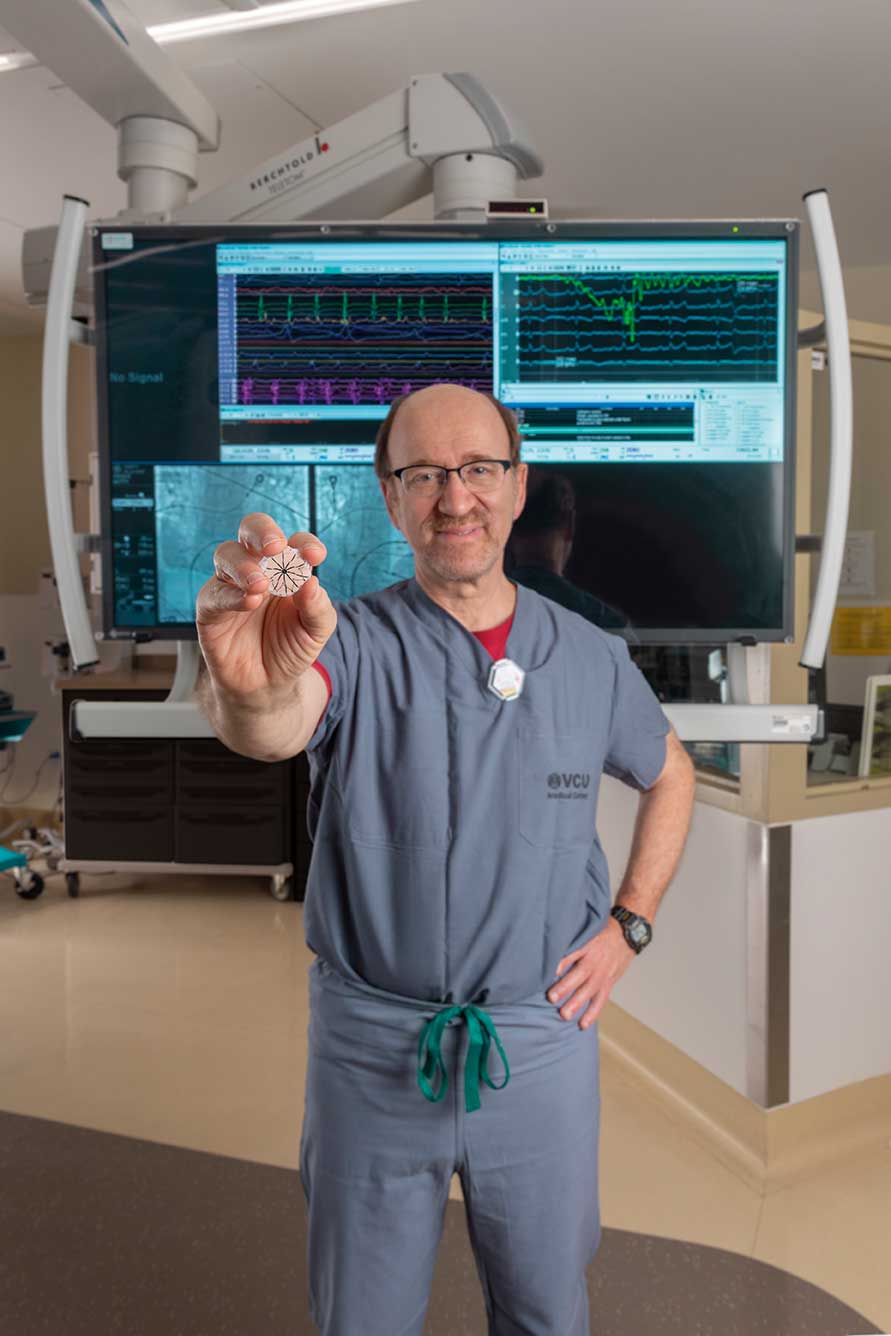
“If you’re on a blood thinner and you start bleeding on an airplane, or on a boat, or when you’re hiking in the woods, that could be disastrous,” said Kenneth Ellenbogen, M.D., the Martha M. and Harold W. Kimmerling, M.D., Chair of Cardiology at the VCU School of Medicine. “Furthermore, if you like playing basketball or going mountain biking, and you’re on a blood thinner, you’d better think twice before doing those things.”
In addition, being on blood thinners means increased risk for internal bleeding in the brain, the gut and elsewhere. Some people even experience chronic bleeding and become very sick over time.
These risks are why Dr. Ellenbogen is studying whether freedom from blood thinners could become a reality for patients with non-vascular AFib who are at high risk of stroke. He is a co-chair of CHAMPION-AF, a global, head-to-head clinical trial of the WATCHMAN FLX device versus non-vitamin K antagonist oral anticoagulants (NOACs).
“This is a groundbreaking study that looks at a device that the doctors here have been implanting for a number of years successfully, and looks at it as first-line therapy for preventing stroke in patients with atrial fibrillation,” Dr. Ellenbogen said. “That’s huge.”
WATCHMAN vs. NOAC
The CHAMPION-AF clinical trial compares NOACswith the WATCHMAN FLX, putting the best available drugs up against the best available left atrial appendage closure device.
“We’re studying different strategies for preventing stroke in patients with atrial fibrillation. And of course, the strategy most commonly used has been drug strategy,” Dr. Ellenbogen explained. “Blood thinners are great, but they make it harder for you to stop bleeding when you start bleeding. So, in patients who have atrial fibrillation, most of their strokes come from what we call the left atrial appendage, which some surgeons call the appendix of the heart. Somebody came up with the idea of if we could close off the left atrial appendage, we might be able to prevent strokes for patients with atrial fibrillation. And they wouldn’t have to take blood thinners.”
In a number of pivotal studies, Ellenbogen said, it was found that patients who can’t take blood thinners but who received the WATCHMAN did well with an aspirin a day, or nothing.
“We have a lot of patients who come to see us who don’t want to take blood thinners because they’re active, or they’ve had some bleeding,” Dr. Ellenbogen said. “This study gives them the opportunity to get a device implanted without having to have had a bleeding episode to get the device implanted. So, if you’re 70 years old and you have high blood pressure, you’re going to be on blood thinners the next 20 years of your life. But if you participate in this study, you have a 50% chance of having a device implanted. So, we can see which is better, the medicine or the drugs.”
After receiving the device, patients will be evaluated in three years. “We’ll be looking to see if this device is safe and effective compared to the drug,” Dr. Ellenbogen said. “If this study proves that the WATCHMAN is as good as or better than blood thinners, then why ever put someone on a blood thinner? We could allow people to live the type of life they want.”
What’s Next?
“This is probably one of the most important studies being done in the next five years in clinical cardiology,” Dr. Ellenbogen said. “I’m going to be involved as one of the two people who is going to steer the study to its conclusion. Whether it’s positive or negative, it’s going to possibly change the way we practice.”
That change could mean that any patient with AFib gets a WATCHMAN device implanted to prevent a stroke. The implant would be in place of drug therapy, which is perfect for active people who have years of full life ahead of them — trips to take, grandkids to raise and races yet to win.
If you are interested in supporting clinical trials and other research that advances lifesaving and life-changing research for people facing atrial fibrillation or other heart arrythmias, contact Carrie Mills, senior major gift officer at VCU Health, at 804-828-0423 or carrie.r.mills@vcuhealth.org.